Herbal Max Gun Power
"Order 30caps herbal max gun power overnight delivery, herbals and surgery."
By: Bertram G. Katzung MD, PhD
- Professor Emeritus, Department of Cellular & Molecular Pharmacology, University of California, San Francisco

http://cmp.ucsf.edu/faculty/bertram-katzung
Patient does not improve or status worsens Focus should be given to other factors including psychiatric cheap 60cap herbal max gun power mastercard wiseways herbals, psychosocial support generic herbal max gun power 30caps with mastercard herbs definition, and compensatory/litigation cheap herbal max gun power 30caps free shipping herbals wholesale. Amended In assessment of patients with persistent symptoms order herbal max gun power 30caps visa vindhya herbals, focus should be given to other factors including psychiatric, psychosocial support, and compensation/litigation issues and a comprehensive psychosocial evaluation should be obtained, to include: a. Mental health history for pre-morbid conditions which may impact current care Not Reviewed, C-2 c. Pre-injury: older age, female gender, low socio-economic status, low education or lower levels of intellectual functioning, poorer coping abilities or less resiliency, pre Not Reviewed, C-3 existing mental health conditions (e. Post-injury: injury-related litigation or compensation, comorbid mental health conditions or chronic pain, lower levels of or less available social support Not Reviewed, C-3 Any substance abuse and/or intoxication at the time of injury should be documented. Deleted Symptom exaggeration or compensation seeking should not influence the clinical care Not Reviewed, C-3 rendered, and doing so can be counter-therapeutic and negatively impact the quality of Deleted care. Not Reviewed, C-3 the unique individual pattern of symptoms should be documented and be the focus of Deleted treatment. An atypical pattern or course (worsening or variable symptom presentation) is Reviewed, C-5 demonstrated Recommendation 21 Amended b. The patient is experiencing difficulties in return to pre-injury activity (work/duty/school) c. Referral to mental health specialty of patients with persistent behavioral symptoms Reviewed, C-5 Recommendation 21 should be considered. Amended Patients who are refractory to treatment of physical symptoms in the initial care setting Reviewed, C-6 Recommendation 21 should be referred to specialty care for further evaluation and management. Amended Patients who have cognitive symptoms that do not resolve or have been refractory to treatment should be considered for referral for neuropsychological assessment. Individuals who present with memory, attention, and/or executive function problems which did not respond to initial treatment (e. It may be necessary or beneficial to meet with other members of Not Reviewed, C-7 the patient?s support system (family, care giver) and/or invite the patient to ask them to Deleted come to an appointment together with the patient. Case managers (in collaboration with the treatment team) should prepare and document Not Reviewed, C-7 a detailed treatment plan in the medical record describing follow-up care and services Deleted required. Case managers may provide assistance to the patient and family who are transferred to Not Reviewed, C-7 another facility (e. Maintain frequent contact by phone to remind about or facilitate an appointment Not Reviewed, C-7 c. Deleted Educational interventions should generally include information and a description of the Not Reviewed, C-7 specific procedures and events the patient will experience at the various phases of Deleted treatment and continue throughout the continuum of care. Open-ended questioning, active listening techniques, eliciting anticipation of future stressors, encouraging the patient to ask questions, and Not Reviewed, C-7 eliciting and encouraging utilization of the patient?s social support resources are Deleted important strategies regardless of whether information-giving or coping skills training interventions are being used. Educational interventions may also include coping techniques for symptom management, Not Reviewed, C-7 such as patient education handouts and helpful tips. Patients may Not Reviewed, C-7 need to proceed through medical or disability evaluation processes. This process should Deleted follow national and local regulations and is beyond the scope of the guideline. A referral to a structured program that promotes community integration may be Not Reviewed, C-7 considered for individuals with residual persistent post-concussive symptoms that impede Deleted return to pre-injury participation in customary roles. The amount of time between visits will vary depending on a number of factors, including the following: a. As soon as the patient is doing well, then follow-up every 3 to 4 months would be recommended iii. Telephone follow-up may be sufficient to evaluate resolution of symptoms and reinforce education c. Veterans Health Administration, Office of Quality & Performance, Evidence Review Subgroup; Revised April 10, 2013. Centers for Disease Control Prevention; National Center for Injury Prevention and Control; Division of Unintentional Injury Prevention. Report to congress on traumatic brain injury in the United States: Epidemiology and rehabilitation. Preventive Services Task Force: Refining evidence-based recommendation development. Society for Medical Decision Making Committee on Standardization of Clinical Algorithms. DoD policy guidance for management of mild traumatic brain injury/concussion in the deployed setting. Evaluation of the military acute concussion evaluation for use in combat operations more than 12 hours after injury. Screening for a remote history of mild traumatic brain injury: When a good idea is bad. The usefulness of brain magnetic resonance imaging with mild head injury and the negative findings of brain computed tomography. A quantitative review of the effects of traumatic brain injury on cognitive functioning. Systematic review of the prognosis after mild traumatic brain injury in adults: Cognitive, psychiatric, and mortality outcomes: Results of the international collaboration on mild traumatic brain injury prognosis. Diagnostic accuracy studies in mild traumatic brain injury: A systematic review and descriptive analysis of published evidence. Advanced topics in neuropsychological assessment following sport-related concussion. Cognitive complaints after mild traumatic brain injury: Things are not always what they seem.
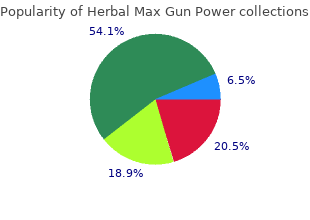
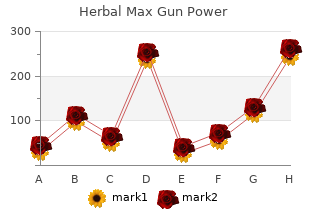
It is useful to assess the patient?s Post traumatic amnesia recall of events following their injury by asking specific questions such as what is their first clear memory buy herbal max gun power 60cap with mastercard jenith herbals, who Persistent post traumatic amnesia is a strong helped them at the scene and how they got to hospital generic herbal max gun power 30 caps with mastercard krishna herbals. A patient who has an early post traumatic seizure to supplement the history? of post traumatic amnesia while in the emergency department would be considered for events discount herbal max gun power 60cap without prescription herbs mopar. They are frequently seen on sporting fields 133 cheap herbal max gun power 30 caps herbals kidney stones, 162, 168, 172, 174 There has been some debate whether and in young children. It has been proposed that these persistent vomiting is more relevant than isolated vomiting. All the major adult clinical decision rules have either that outcome was universally good for these concussive vomiting or recurrent vomiting as a major risk factor for convulsions? in elite Australian sportsmen. In the paediatric literature recurrent or focal post traumatic seizures are more likely to be vomiting is also considered a significant risk factor although associated with significant intracranial injury. Some patients it is noted that isolated vomiting is more common in who have seizures associated with trauma may have pre younger children. Clement et al77 identified any vomiting existing epilepsy which may either have caused the seizure as a significant risk factor for neurosurgical intervention in or resulted in a lower seizure threshold. Mild headache is a common decision rule because of their perceived clinical importance. Interestingly, in a early rapid reversal of warfarin in patients with intracranial later study, Clement et al77 found that severe headache was haemorrhage significantly improved mortality. Mild head injury patients who are warfarinised are at significantly increased risk of traumatic intracranial the general trend of the literature would suggest that mild haemorrhage particularly if they are elderly or over headache is not a significant concern but persistent severe warfarinised. Note that this increased risk applies to headache should be considered a significant risk factor for asymptomatic patients. Mina injury, it would be reasonable to postulate that increasing et al147 demonstrated that pre-existing anticoagulation age and the presence of more than one anti-platelet agent significantly increased the risk of death from intracranial would increase the risk of bleeding. Subsequent small studies by Franko et al,78 Ivascu present this remains unknown and prolonged observation et al,79 Cohen et al,148 Fabbri et al41 and Allard et al149 and close follow up in the community is probably prudent. Similarly, in mild head injury as they could not identify any useful clinical the paediatric literature, abnormal mental status has been predictors of intracranial injury in the elderly. Clinical observation of alertness, intracranial risk with age and that occult presentation was behaviour and cognition will detect more subtle changes more common. It is worth noting that the hours post injury and certainly by four hours post injury. Large non scan is not available and the patient has no other identified frontal scalp lacerations have been identified as significant risk factors in young children. Haydel et al32 identified visible trauma above the clavicles? Abnormal alertness, behaviour or cognition as a major risk factor. Mower et al58 identified scalp haematoma as a major risk factor and included it in their Persistent abnormal mental status manifested by 47 clinical decision rule. There is injury because it manifests as abnormal mental status which no evidence for the use of descriptors such as boggy? or impairs clinical assessment and must be assumed to be tense? to help discriminate between significant and non due to intracranial injury. Cook et al,60 in a study of alcohol intoxicated 20, 38, 60, 72, 88, 115, 162, 172, 174 required. In studies on patients with mild have suggested that drug or alcohol intoxication is a risk head injuries, specific high risk factors for intracranial injury factor for intracranial injury but the exact definition of that have been identified include focal blunt trauma to the intoxication remains vague. Although it would unstable vital signs or associated injuries requiring appear that alcohol intoxication is not an independent significant amounts of analgesia, procedural sedation risk factor for intracranial injury it remains a common 162, 172, 174 or general anaesthesia. From a practical significant features such as prolonged loss of consciousness viewpoint, any pre-existing medical condition resulting or seizures. Clinical judgement is exhaustive systematic literature search but represents the required. Patients who present more than four hours most relevant studies identified by the author. Maguire et al86 published patients who presented more than 24 hours post injury a systematic view of paediatric clinical prediction rules or who represented, so there is a lack of evidence about in 2009 that assessed all the major studies except the these patients. The studies by Dunning et al enrolled studies that patient?s who have persistent or new abnormal 22,772 patients and Kupperman et al enrolled 42,412 mental status, or persistent or new clinical symptoms such patients and these are the two largest well designed studies as vomiting or severe headache, have increased risk of yet performed on either adult or paediatric patients with intracranial injury. In their summary of their clinical presumed that appropriate care could be delivered in the decision rule, they included their figures on the percentage event of deterioration. Prolonged clinical observation for at least 24 hours, associated with clinical improvement, has been shown to make a significant injury unlikely in the majority of mild head injury patients. The exception would be is identified, further management should be discussed elderly patients who are anticoagulated who are at risk of with a neurosurgical service including measures to reduce delayed subdural haemorrhage. When can patients with mild head injury be safely discharged and what discharge advice should be provided? Clinical criteria: A Normal mental status (alertness / behaviour / cognition) with clinically improving minor post concussion symptoms after observation until at least four hours post injury. Written and verbal head injury discharge advice should be given to the patient and a nominated A responsible person covering: symptoms and signs of acute deterioration reasons for seeking urgent medical attention lifestyle advice to assist recovery typical post concussion symptoms reasons for seeking further medical follow up. In both high and low risk mild head injury observation after initial period of in-hospital observation if patients, potential clinical indications for admission such they meet clinical, social and discharge advice criteria. Whatever the period of observation selected, 174, 178, 181, 184, 191 Mild head injury patients can be safely the provision of safe discharge advice and assessment discharged from hospital for home observation when the of the patient?s social situation is mandatory because risk of acute deterioration from an underlying intracranial occasional cases of deterioration following discharge are injury is assessed as being low. An example of a suitable head injury discharge requires that the patient has adequate social supports and advice sheet is attached at Appendix 6.
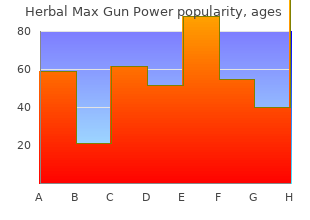
If the obstruction does not resolve with this treatment buy generic herbal max gun power 30 caps herbs collinsville il, endoscopic balloon dilation of long-standing anastomotic strictures or short strictures not associated with fistulae can be attempted buy generic herbal max gun power 30 caps line herbs meaning. However cheap herbal max gun power 30 caps herbalism, surgical intervention (either resection or stricturoplasty) is preferable buy 30 caps herbal max gun power rumi herbals pvt ltd. Stricturoplasties are especially useful in the duodenum, for jejunoileitis, and to preserve bowel length in patients who have undergone previous bowel resections (Figure 23). Fistulae often tract through the mesocolon and may enter the small intestine or vagina. Long-standing inflammation often results in scarring and fibrosis and consequently in bowel obstructions. Although most strictures are benign, stricture formation may reflect carcinoma in chronically diseased intestinal segments. Medical management of patients with Crohn?s colitis begins with dietary modification to eliminate foods that stimulate bowel activity (dairy products and highly seasoned food). Initially medical therapy consists of sulfasalazine, corticosteroids, and aminosalicylates orally or as retention enemas. In refractory cases, metronidazole and azathioprine or 6-mercaptopurine are added. Cyclosporine is an additional immunosuppressive for those patients with intractable disease. Other indications include inability to sustain clinical remission, or the management of complications such as fistula, abscesses, obstructions, and cancer. Proctocolectomy with Brooke ileostomy is the conventional treatment for Crohn?s colitis with rectal involvement (Figure 24). In cases of Crohn?s colitis with rectal sparing, colectomy with ileorectal anastomosis is the procedure of choice (Figure 25). Isolated segments of Crohn?s colitis may be treated with segmental colectomy and anastomosis. Perianal Disease Anal fissures, as well as ulcers in the anal canal resulting in perirectal abscesses or fistulae, are a difficult complication of Crohn?s disease. The fistulous openings are commonly in the perianal skin but may also appear in the groin, the vulva, or the scrotum. Perianal abscesses present with pain exacerbated by defecation, sitting, or walking. Fever may be the sole presenting symptom or it may accompany redness and pain in the perianal region. Severe persistent perianal disease leading to repeated surgical procedures can result in anal sphincter destruction and fecal incontinence. Therapy for perianal disease should be aimed at the relief of symptoms and the preservation of the anal sphincter. Sitz baths for local cleansing should be included in the first therapeutic measures along with antibiotics. Efforts should be made to minimize intestinal disease activity because successful management of the disease process reduces episodes of diarrhea passing through the perianal area. A trial of metronidazole or ciprofloxacin may be helpful, although discontinuation of the drug results in recurrence of perianal disease in many patients. Remicade has led to healing of fistulae in 50% of patients and improvement in 60%. A number of surgical approaches may be performed if drainage and medical therapies are not successful. Surgical drainage with seton placement and placement of mushroom catheters, which may be left in place for prolonged periods during the healing process, have been successful. Alternative approaches include partial internal anal sphincterotomy to remove cryptoglandular epithelium as well as fecal diversion by colostomy. Neoplasia Like ulcerative colitis, the risk of colonic neoplasia in patients with Crohn?s disease is a recognized complication of the disease. The risk of colon cancer appears to be related to the severity and the duration of the disease, the age at disease onset, stricture formation and the presence of primary sclerosing cholangitis. Unlike ulcerative colitis, there are no standardized guidelines for surveillance in Crohn?s disease patients. However, in those patients with Crohn?s Disease for 8?10 years, colonoscopic surveillance should be undertaken at 2?3 year intervals and at 1?2 year intervals for patients with a disease history of over 20 years. Dysplasia is the precursor to cancer in these patients and therefore a total of 30 biopsies are recommended at 10-cm intervals throughout the colon. If there is a stricture, a pediatric colonoscope may allow examination of the bowel proximal to the stricture. Patients with indefinite dysplasia should receive aggressive therapy to control inflammation. Finding dysplasia on surveillance colonoscopy is sufficient to recommend surgical intervention (colectomy). New drugs, nutritional therapies, advances in surgical techniques, improved postoperative care, and recognition of cancer risk have improved the outlook. In particular, stricturoplasties are used to prevent short-bowel syndrome, a severe malabsorption syndrome resulting from repeated long resections. Patients with short-bowel syndrome may require long-term home parenteral alimentation or even a small-bowel transplant.
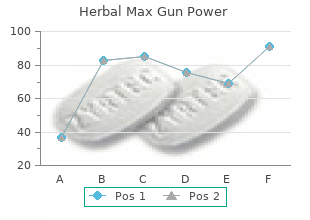
Syndromes
- Abdominal pain
- An adult with who has fewer than 1700 neutrophils in a microliter of blood has a low white blood cell count.
- Nosebleeds (epistaxis)
- Feeding problems
- Your surgeon removes any small disk fragments, bone spurs, or other soft tissue.
- Have difficulty breathing
Indirect detection methods can provide valuable additional diagnostic information since blood cultures are less sensitive and because pertinent purchase 60cap herbal max gun power visa herbals outperform antibiotics in treatment of lyme disease, invasive diagnostic testing in culture of the organ candidiasis is often not possible when there is severe immunosuppression purchase herbal max gun power 30caps online herbals that lower cholesterol. Both antigen and antibody detection methods are available to serologically diagnose invasive fungal infections buy discount herbal max gun power 30 caps herbals images. However herbal max gun power 30 caps for sale herbs nyc, it should be noted that the clinical interpretation of serological test results can be problematic [348]. An acute infection is indicated by the positive detection of antigens as well as high or rising (whole) antibody titers. The literature has indicated that Candida-IgA and IgM antibody titers are especially elevated during an acute infection [243]. An infection is suspected in agglutination tests when titers are between 16 and 32 and there is a normal peripheral neutrophil count. False positive results occur, for example, when there are existing rheumatoid factors or limited kidney function. The amount of detectable mannan is, however, not the same for individual Candida species due to the antibodies used in the test. The results of mannan antigen detection are inadequate, particularly for infections with C. The disadvantages of the different test systems for detecting antigens are the low sensitivity, particularly with the agglutination methods, and the often false-positive results. Based on the observation that often no mannan antigens can be detected when there are high Candida mannan antibody levels, and by the same token, high mannan antigen values are observed when the Candida mannan antibody levels are low, the literature suggests using a combined mannan antigen and mannan antibody test [214]. Since Candida yeasts often occur in healthy individuals as commensal organisms, a reliable differentiation between superficial colonization, mucous membrane thrush and invasive organ candidiasis has its limitations. A further problem is that the formation of antibodies is often absent when there is severe immunosuppression. In commercial test systems, poorly characterized mixed antigens are often used which sometimes stem from different C. The result is that classic antibody detection methods can only be used to a limited extent to diagnose invasive processes, especially with severely immunosuppressed patients. Tests performed during the course of the infection are recommended in order to better assess the results of Candida antibody detection tests. Even though there are scientific indications that combining different Candida antigen and antibody detection tests increases the quality of the serological diagnostic testing for invasive candidiasis, this has yet to be backed up by reliable clinical data. At the same time, the significance of Candida serology for estimating the necessary length of treatment still needs to be sufficiently evaluated. As a result, expert societies have not given any official opinion statements on using a step-wise approach for the serological diagnostic testing of Candida. Neither the national recommendations nor the international guidelines have touched upon the issues of when is the right point in time to conduct serological tests, the optimum frequency of serial tests, the significance of class-specific detection of Candida antibodies and the suitable combination of various biomarkers [66; 273]. Due to the identified uncertainties in the serological testing for Candida, serological findings should always be compared with other diagnostic measures and the clinical picture. A diagnosis of Candida infections and a treatment decision based solely on serological parameters should not be made. No reliable differentiation can be made between colonization, superficial skin/mucous membrane infections and deeper organ candidiasis using only serodiagnosis. At the same time, serological testing for Candida is not suitable for differentiating between species. See MiQ 5 for an evaluation of Candida serology in the context of other diagnostic measures [348]. Isolated autochthonous infections in Europe are proof of the increasing distribution of C. Cryptococcosis is primarily an infection in individuals with compromised immune systems. The primary stage is usually devoid of clinical symptoms and can lead to chronic endobronchial colonization, solitary lung mycosis (cryptococcoma) and pneumonia (primarily caused by C. In patients with T cell defects, cryptococcosis clinically manifests after hematogenous spread and the manifestation index for C. All parenchymatous organs, bones and joints (the latter in around 7% of cases) can be affected. Due to the neurotropism of Cryptococcus, disseminated cryptococcosis most commonly 220 manifests in the central nervous system. Patients develop headaches and other symptoms of a basal meningitis or meningoencephalitis, possibly even mental alterations. Patients undergoing tacrolimus treatment after an organ transplant display another clinical picture for cryptococcosis. Primary cutaneous cryptococcosis caused by a traumatic pathogen inoculation constitutes its own clinical entity and must be differentiated from a cutaneous manifestation caused by hematogenous spread since the treatment and prognostic consequences differ. Due to insufficient scientific data, no general statement can be made about sensitivity and specificity. In the case of a disseminated cryptococcosis, antigen concentrations are usually highest in serum, and higher in liquor than in urine. A serum sample should always be tested parallel to antigen screening in liquor because disseminated cryptococcosis cannot be ruled out even if no antigens are detected in liquor. According to manufacturer specifications, antigen detection limits fluctuate between?
Purchase herbal max gun power 30caps mastercard. Planting Herbs in Containers: Oregano Chives Thyme Mints Basil Sage Rosemary Lavender.

