Glyburide
"Cheap glyburide 5 mg amex, diabetes in canines signs."
By: William A. Weiss, MD, PhD
- Professor, Neurology UCSF Weill Institute for Neurosciences, University of California, San Francisco, San Francisco, CA

https://profiles.ucsf.edu/william.weiss
In contrast buy 2.5mg glyburide amex diabetes type 2 life insurance, cases where the placenta eventually migrated away from the internal os discount 5 mg glyburide free shipping managing diabetes 33, the observed mean rate of migration was 4 cheap 5 mg glyburide mastercard diabete type 1. Placen tal edge overlapping the internal os at the mid-trimester scan cheap glyburide 2.5mg on-line diabetes diet, and a thick placental edge (where the angle between the placental edge and the uterine wall is less than 135o) are known to be associated with reduced likelihood of placental migration. If the placental edge is overlapping, the internal os or is within 2 cm on l In cases with asymptomatic major placenta praevia, transvaginal scan at 38 weeks, elective caesarean section is a transvaginal ultrasound scan should be performed at reasonable (Fig. The bleeds are thought to occur due to the formation of term will not be encountered unless the placental edge is at the lower uterine segment. Fetal malpresentation or unsta least reaching the internal cervical os at mid-pregnancy. Many women Transvaginal ultrasound is safe in the presence of placenta with major placenta praevia do not bleed until the onset of praevia, and is more accurate than transabdominal ultra labour. Ultrasound is useful to observe and document the phenomenon of placen Management tal migration from the lower uterine segment. It is widely believed that this process is not a true migration of placental the management of placenta praevia depends upon clinical tissue. Anticoagulation to reduce the risk of clots should be reserved for those women at a particularly high risk of thrombosis, and regular unfractionated heparin should be preferred due to its short duration of action. Traditionally, caesarean section has been the recom mended mode of delivery for major placenta praevia, whereas for minor praevia an attempt at vaginal delivery was considered appropriate. Until recently, no evidence based protocol was available for management of delivery guided by the fndings of the ultrasound scan. We reported that in cases where the placental edge was within 1 cm of the internal cervical os within 2 weeks of delivery, all women required a caesarean delivery due to bleeding. Initial it is recommended that these cases be still referred to as haemorrhages called warning haemorrhages are often low-lying placenta. Vergani and colleagues reported that needed for severe, intractable or recurrent bleeding. Fetal more than two-thirds of women with a placental edge to morbidity is because of iatrogenic prematurity. Placenta edge-internal os distance was measured up raphy should be performed in these women. Women be possible even for those women with placental edge to with major placenta praevia, who have previously bled internal os distance of 1. Prospective studies in historically, are admitted and managed as in-patients from which the distance was measured closer to the time of birth 34 weeks of gestation. Constant company of an adult and the guidelines also recommend that any women going to full-informed consent of the pregnant woman are required the operation theatre with known major placenta praevia for home-based care of women with major placenta prae should be attended by an experienced obstetrician and an via. This is especially true if these women also have the event of abdominal pain or vaginal bleeding. Prior to the previous uterine scars, an anterior placenta or are suspected delivery a discussion about the delivery plan, risks of severe to be associated with placenta accreta. Four units of cross haemorrhage, need for blood transfusion and the possibility matched blood should be kept ready, even if the mother has of surgical intervention including removal of the uterus never reported vaginal bleeding. Gentle choice of anaesthetic technique for caesarean sections is mobility and the use of elastic compression stockings usually made jointly by the anaesthetist, the obstetrician 156 Practical Guide to High-Risk Pregnancy and Delivery and the pregnant women. The timing of surgery should be A causal relationship between hypertension and abrup deferred till 38 weeks if possible in order to reduce neonatal tion is not completely proven. It occurs in sels as in normal pregnancy, and the lack of trophoblastic approximately one in 80 deliveries and remains a signif invasion of uterine vessels. Pathology and Aetiology Clinical Presentation the precise cause of abruption is unknown. Abruption arises from haemorrhage into the decidua basalis of the the diagnosis of placental abruption is clinical, based on placenta. This results in the formation of haematoma and an characteristic signs and symptoms. This is then con increase in hydrostatic pressure leading to separation of the frmed by evaluation of the placenta after delivery on adjacent placenta. The resultant haematoma may be small gross examination of the placenta, which reveals a clot and self-limited or may continue to dissect through the and/or depression in the maternal surface. That releases thromboplastins and bleeding of abruption are tense, tender and/or irritable uterus (this into myometrial layers (Couvelarie uterus). This damage may be less obvious if posterior placenta), signs of shock interferes with uterine contractility, causing atony predis which are out of proportion to estimated blood loss posing postpartum haemorrhage. However, the bleeding (concealed abruption), frequent uterine contractions on may be in completely or partially concealed, if the haema tocograph suggestive of uterine irritability with or toma does not reach the margin of the placenta and cervix, without associated fetal heart rate abnormalities on the the blood loss may not be revealed. Ultrasound is an insensitive and unreliable tool for detecting or excluding placental abruption, as negative sonographic fndings are common with clinically signifcant abruptions. Low birth-weight, fetal growth restriction, Increasing parity neonatal anaemia and hyperbilirubinaemia are signifcantly Presence of multiple gestations more common. In cases presenting with the fetus Polyhydramnios still alive, fetal heart rate abnormalities are common. A Trauma marked elevation in stillbirth rate is observed if the separa Possibly thrombophilias tion exceeds 50% of the placental area. Treatment consists of initial Chapter | 10 Antepartum Haemorrhage 157 mother and fetus.
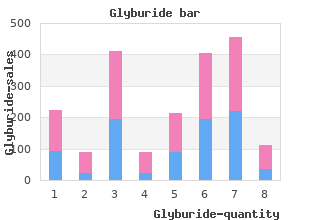
Platelets Thrombocytopenia is relatively common in pregnancy and may represent either benign or pathological conditions which require diagnosis and follow up order glyburide 5 mg with visa blood sugar zippy. Rubella immune Record Rubella status as immune (positive titre) or nonimmune (negative or indeterminate) generic 2.5 mg glyburide overnight delivery diabetes urine test strips for dogs. The information is important for assessment of maternal liver function and identifying newborns that require Hep B immunoprophylaxis after birth cheap glyburide 2.5mg otc diabetes test empty stomach. Consider rescreening those at risk of acquiring syphilis during pregnancy in each trimester cheap glyburide 2.5 mg free shipping diabetes prevention trial type 2. Consider rescreening those at risk of acquiring gonorrhoea during pregnancy in each trimester. Consider rescreening those at risk of acquiring chlamydia during pregnancy in each trimester. Consider re-screening if the first screen is positive or there is a history of recurrent urinary tract infections. Repeat Antibodies Done for those who are Rh(D) negative prior to administering Rh(D)Ig. Additional investigations as these tests should be considered when clinically indicated, often at indicated: the time of the first trimester lab tests. The availability of prenatal genetic investigation should be discussed early in the pregnancy, as the information is complex and the tests are time specific. Document the test(s) selected, if testing was declined or if screening was not feasible due to being outside the appropriate gestational age. This test can be initiated as early as 9-10 weeks� gestational age and up to any gestation. Consider discussing this option with all patients/clients, even if the gestational window for standard testing has elapsed. Abnormal Placental Abnormal serum markers may reflect abnormalities of placentation Biomarkers and require further follow up. Anatomy scan (between the anatomy scan is also a genetic screening test which can detect 18-22wks) major and minor malformations of the fetus. Placental Location Document the location of the placenta as noted on the ultrasound Soft Markers Soft markers are obstetric ultrasound findings that are considered variants of normal but are associated with varying degrees of increased risk for underlying fetal aneuploidy. In women with a low risk of aneuploidy following first trimester aneuploidy screening, the presence of specific ultrasound �soft markers� associated with fetal trisomy 21 (echogenic intracardiac focus) or trisomy 18 (choroid plexus cysts) identified during the second trimester ultrasound (18 to 22 weeks) is not clinically relevant due to poor predictive value. With the exception of increased nuchal fold, they should not be used to adjust the a priori risk for fetal aneuploidy and do not warrant further testing [34]. Genetic screening result this is a prompt to remind care providers of the importance of reviewed with pt/client reviewing the genetic screening results with the pregnant person to ensure they understand results and potential next steps. Plan of management/ For each issue identified, indicate follow up plans affecting antenatal, Medication change/ intrapartum, postpartum and newborn care. This may include Consultations consultations, investigations, results and medication changes. There is continuing research into the optimal dosage and some specialists use higher doses � consult with your local referral centre for advice. Risk factors include, but are not limited to, a history of preterm birth or a shortened transvaginal cervical length < 2. This decreases the risk of clinical lesions and viral shedding at the time of delivery and therefore decreases the need for a caesarean section. Include the date the swab was done, results and sensitivities Other indications if indicated. These are indications for intrapartum Y/N antibiotic prophylaxis and negate the need for a rectovaginal swab. Item Description Rh(D) neg [ ] Non-sensitized Rh(D) negative pregnant people should receive Rh(D) immunoglobulin at 28-29 weeks� gestation. As Rh(D) immunoglobulin is a blood product, usual practice for discussion and consent should be followed. This is administered as a three dose series and is available free of charge from the local Public Health Department. Measurement of urinary protein by dipstick (ranges from neg (-), trace (tr), 1+, 2+, 3+, 4+). There are conflicting guidelines about the utility of routine screening for urinary protein. However, it has been left on this form until up-to-date Canadian clinical practice guidelines are issued. This measurement is operator-dependent and if 26 Ontario Perinatal Record User Guide | Update: August 2018 possible should be performed by the same provider with consistency in the positioning the patient. Fundal height in cm correlates approximately to gestational age in weeks but is affected by fetal position and habitus of the pregnant person. Presentation refers to the fetal anatomical part closest to the pelvic inlet (usually the head or the buttocks). This box may be left blank in early pregnancy visits until fetal parts are more easily palpated. Document rate when at risk for heart rate anomalies or when auscultation reveals a rate outside the normal range of 110-160 bpm. Comments Refers to any additional information relative to the condition of the patient/client and fetus. Next Visit Indicate the interval until the next visit and any upcoming tests or procedures.
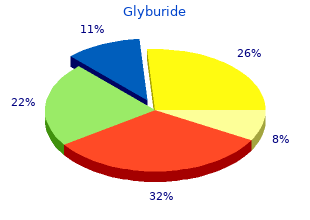
Household and family members and others who are likely to effective glyburide 2.5 mg diabetic blood sugar chart have close contact with babies should also ensure their pertussis vaccination is up-to-date order glyburide 2.5mg overnight delivery diabetic acidosis. However generic 2.5mg glyburide with visa diabetes insipidus diagnosis, where vaccine has inadvertently been given during pregnancy buy glyburide 5mg with amex diabetes prevention guide, further doses should be deferred until after delivery. Influenza Annual flu vaccination is recommended for all adults, and especially smokers, those with chronic diseases, those over 65 yrs. Pregnant women should be actively encouraged to have the flu vaccine which can be given at any stage during pregnancy. Fact sheets about these vaccinations, a pre-vaccination check list, and possible reactions to vaccinations are available at the practice. This is an individualised growth chart for the mother and has been shown to improve screening for growth restriction or macrosomia. It is important that the symphysio-fundal height is plotted on the chart at each visit. If a growth chart has not been developed for the woman, please contact the Women�s Health Clinic and we will create one and fax it to you. The first trimester screening involves nuchal translucency at 11 � 13w6d and biochemistry from 9w0d 13w6d. It is imperative that all the information required on the first or second trimester serum screen request form is filled in as it has a significant influence on the aneuploidy risk assessment outcome. Women who have an increased risk of a chromosomal disorder or those with a family history of genetic disorder should be offered the first trimester screen or referred to the Prenatal Diagnosis Clinic early for appropriate counselling. Maternal Age Maternal age is a poor screening test Offering diagnostic testing to all women over 37 years will detect less than 50% of babies with Down Syndrome, and will expose an unacceptably high number of pregnancies to the miscarriage risk associated with invasive diagnostic testing. This also applies to all pregnant women of any age as most of the aneuploidies detected in pregnant women are from the younger age group. Nuchal translucency alone Measured between 11 � 13+6 weeks Not as accurate as combined first trimester screening Good option if patient doesn�t manage to get blood taken by 13+6 weeks Good option for twin/multiple pregnancies 4. The 18 � 20 week morphology scan Not recommended as a screening test for Down syndrome specifically but the detection of soft markers should prompt referral to the Prenatal Diagnosis or High Risk Clinic for further discussion. Some women will be satisfied with a risk of eg, 1:250, particularly if this is significantly lower than their age-related risk or if they decide against invasive testing. Women who receive screening results before 14 weeks will have a choice between the two. Women who receive screening results after 14 weeks will only have the option of amniocentesis. Transvaginal procedure is not usually performed because of the significant increased risk of miscarriage. Terminations of pregnancy after around 14 weeks are carried out by inducing labour. Usually requires clarification by amniocentesis (mosaicism can be confined to the placenta). Wait for the 18 � 20 week ultrasound Ultrasound is a poor screening test for Down syndrome on its own, as approximately half of all fetuses with Down syndrome will have completely normal morphology scans. However, ultrasound can be useful in the context of an �increased risk� screening result. Time is then running out for termination of pregnancy if diagnostic testing is performed and yields abnormal results. Counselling of Those Screening �At Increased Risk� of a Chromosomal Disorder Patients who receive an �increased risk� screening result should be offered a face-to-face appointment to discuss the result. The person counselling the patient should aim to cover the following: Address anxiety Assess understanding of what Down syndrome is Discuss magnitude of screened risk relative to patient�s age-related risk Outline options (no action/diagnostic testing/wait for 18-20 week ultrasound) including advantages and disadvantages of each Explain the diagnostic procedures, what�s involved, risk of miscarriage Explain limitations (a normal karyotype doesn�t rule out all genetic diseases) Explore patient�s thoughts about raising a child with a disability (resources & support � financial, emotional and family) Explore patient beliefs concerning termination of pregnancy Explain termination procedures (surgical evacuation, induction of labour) Time frame for results the possibility of detecting an unexpected chromosomal abnormality It is preferable that there is a time interval of at least 24 hours between this counselling and any appointment for a diagnostic procedure to allow the patient time to absorb the information, reflect, discuss with their partner, and reach a decision they are comfortable with. If you would like your �increased risk� patient to see a genetic counsellor for discussion and help with decision making, please contact the genetic counselling service (ph. Your patient will be contacted within 24 hours (weekends excepted) and offered a face-to face appointment (although some patients prefer to receive this counselling by phone). Those who elect to await the outcome of the 18 � 20 week scan will be followed up by a genetic counsellor after the scan takes place. Normal results from diagnostic testing will be phoned to the patient by either a genetic counsellor or midwifery staff depending on the route of referral. All abnormal results will be phoned to patients by a genetic counsellor or midwifery staff, and an appointment arranged with a consultant obstetrician (usually) within 24 hours. If your patient is requesting pre-natal diagnosis because of a personal or family history of a single gene disorder or familial chromosomal translocation, please refer directly to the genetic counsellors as soon as possible � some �work-up� may be required before pre-natal testing can be offered. It is a very accurate screening test particularly for Trisomy 21 and 18 and for the sex chromosomes but less so for Trisomy 13. A negative test for the above will mean that the risks of Trisomies 21 and 18 are low. However, if the test does not exclude any of the Trisomies, further invasive testing will need to be carried out to confirm or exclude the diagnosis. It is not funded under Medicare and women will have to pay for the test, which currently costs around $900, but the price is anticipated to come down significantly in the future. The following information therefore relates only to women who are Rh D negative and have no preformed antibodies. This includes: Anti-D administration if a sensitising event occurs in pregnancy; routine prophylaxis at 28 and 34 weeks gestation; and further prophylaxis after birth if the baby is not Rh D negative. This is to cover any and all occasions on which Anti-D may become indicated during pregnancy. These include: any uterine bleeding in pregnancy ranging from (threatened) miscarriage to antepartum haemorrhage; any abdominal trauma in pregnancy; and any uterine or intra-uterine intervention (such as external cephalic version, amniocentesis, etc). If a woman has a sensitising event after routine prophylaxis at 28 weeks, she should have a dose of Anti-D regardless of when the prophylactic dose was administered.
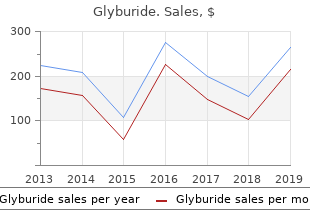
Syndromes
- Pseudomonas aeruginosa
- When writing the contract, take into account all the driving issues that are likely to come up.
- Vomiting or diarrhea
- Delirium
- Prunes
- Fracture of an elbow or other joint
- Headache
Early in the newborn period glyburide 5mg overnight delivery diabetes treatment using stem cells, help asking visitors to cheap 2.5mg glyburide amex diabetes mellitus y obesidad leaveit babies eat frequently buy 2.5mg glyburide with visa diabetes youth families, and nd com works! Learning how to buy 2.5mg glyburide otc blood sugar levels feed your in Whatever your wishes, it is our goal fant can be easier when you learn to to provide you with the best possible read your baby�s early hunger cues care while preparing you to care for and sleep/awake states. Please let us baby with you helps you learn how to know how we can best assist you. All rights reserved To further meet the needs of all patients and families, the Cleveland 116 114 Skin-to-Skin Contact for You and Your Baby What is meant by �skin-to-skin� Skin-to-skin means your full-term, healthy baby is placed belly-down, directly on your chest, right after birth. Your care provider dries your baby off, puts a hat on him or her, covers him or her with a warm blanket, and gets your baby settled on your chest. The rst hours of snuggling skin-to skin let you and your baby get to know each other. If your baby needs to meet the pediatrician rst, or if you deliver by c-section, you can unwrap your baby and cuddle shortly after birth. Newborns crave skin to-skin contact, but it�s sometimes overwhelming for new moms. Eight different research studies have shown that babies who have had the benet of skin-to-skin breastfeed better. The American Academy of Pediatrics recommends that all breastfeeding babies spend time skin-to-skin right after birth. Keeping your baby skin-to skin in the rst few weeks makes it easy to know when to feed your baby, especially if your baby is a little sleepy. A smooth transition Your chest is the best place for your baby to adjust to life in the outside world. Compared with babies who are swaddled or kept in a crib, skin-to-skin babies stay warmer and calmer, cry less, and healthier blood sugar levels. Researchers have watched mothers and infants in the rst few days after birth, and they noticed that skin-to-skin moms touch and cuddle their babies more. Even a year later, skin-to skin moms snuggled more with their 115 117 babies during a visit with the pediatrician. Notes Skin-to-skin beyond the delivery room Keep cuddling skin-to-skin after you leave the hospital. Your baby will stay warm and comfortable on your chest, and the benets for bonding, soothing, and breastfeeding will likely continue. If your baby is sleepy, skin-to-skin can help keep your baby interested in nursing. Babies are comforted by skin to skin during procedures Skin-to-skin may enhance brain development. Fathers and mothers who hold babies skin to skin are thought to have increased condence and are more relaxed. All rights reserved Index# 15276 116 118 Breastfeeding: the First Weeks Getting started the rst weeks of breastfeeding are a learning time for you and your baby. You are learning how to care for and feed your baby, and your baby is discov ering how to breastfeed and ask for comfort. A nurse or lactation consultant will observe you and your baby breastfeeding before you leave the hospital. During the rst weeks, your milk will change from colostrum (a thick, rich uid) to mature milk (a thinner, whitish uid). A Good Start with Breastfeeding � We encourage you to put your baby to breast after birth. Offer your breast whenever your baby shows feeding cues such as mouthing, lip smacking, turning toward the breast, sucking on sts. Feeding on cue or on demand will assure good milk supply because baby�s nursing drives the milk supply. For this or under your arms to support your position, your baby is supported on a baby and avoid straining your back. If you are in pain, take medicine be fore breastfeeding to help make you Pillows should also support both more comfortable. Do this by gently close to you as possible, skin-to-skin placing your hand behind your contact is best. The palm comfortable for both you and your of your hand is placed between your baby. As you pre pare to latch on your baby, be sure Cross-Cradle Position your baby�s mouth is very close to your nipple from the start. When baby opens his/her mouth wide, you push with the palm of your hand from between the shoulder blades. Your baby�s mouth will be covering at least a half inch from the base of your nipple. Most newborns are very breast and four ngers underneath, comfortable in this position. It also away from the dark area around helps when a mother has a forceful the nipple (areola). Your baby�s head will rest in the bend of You support your breast with a "C" your arm, with your forearm sup hold.
Cheap 2.5mg glyburide free shipping. Reverse Diabetes Drink.

